“You have to see what is happening in Okrika,” said Umahi Godwin, a medical doctor and our colleague at the Elizabeth Glaser Pediatric AIDS Foundation (EGPAF).
We are in Nigeria to document transformative programs to end AIDS in children and have come to Rivers State, in the south-south, along the Niger River delta. The many intersecting rivers literally feed the economy of the region, with tilapia, catfish, and Nile perch. In addition, 60% of the nation’s petroleum is refined in industrial cities like Port Harcourt.
Rivers State carries one of the highest HIV burdens in Nigeria, with more than a quarter of those living with HIV in the state not adhering to lifesaving antiretroviral (ARV) medication, in addition to high risk behaviors. With the oil and gas industries, many people migrate within the state and from neighboring states to find work, which can make continuity of health services difficult.
Okrika is a fishing community, which presents a further challenge when it comes to public health—with people often close to the water, but far from health centers and lacking money for transportation. This challenge is that much greater when it comes to babies and children, 80% of whom cannot survive HIV past the age of 5 without ARV intervention.
Dr. Umahi—who is the senior technical officer of Pediatric and Adolescent HIV Service—tells us that Rivers State has the highest estimated number of children living with HIV in Nigeria. Staff at Okrika Zonal Hospital have made a commitment that no child should die of AIDS-related illness within their service area. So the three of us headed out to see how these health workers are reaching babies.

I Am Blessed
I Am Blessed
As our car swings through the gates of the hospital, we hear joyous voices and handclaps echoing into the carpark. We disembark, and a health worker greets us, inviting us to join an antenatal support group that has just started.
The hospital assembly room feels like a church, with the head nurse leading more than a dozen women in energetic hymns about breastfeeding and HIV prevention. “I want to be alive, I want to see my baby, I don’t want to lose my baby, oh Lord, see me through,” sing the women.
This is emotional stuff. Lives are literally at stake for these expectant mothers—their own lives and the lives of their unborn children.

After ten minutes of enthusiastic harmony, the head nurse leads the women in a final, thunderous chorus: “I am blessed! I am blessed! I am blessed! I am blessed!” She then launches into her clinical lesson, sharing health advice, including specific guidance about HIV.
“As we prepare you to be ready for your baby, we also check you for HIV,” she says. “Anyone who is HIV-negative, we counsel them on how to remain negative. Anyone who is positive for HIV, we counsel her to start taking the drugs to treat herself and to protect her baby.”
The nurse dispels common myths about HIV and instructs the women on how they can avoid acquiring the virus and how they can avoid transmitting it to their children. Her advice is frequently punctuated with claps of agreement. She wraps up with a final exhortation to the women to eat nutritious meals and drink enough water throughout the day.
Then the expectant mothers’ queue for antenatal care: to check vital signs, monitor the unborn babies, receive personal HIV counseling and testing, and other services.
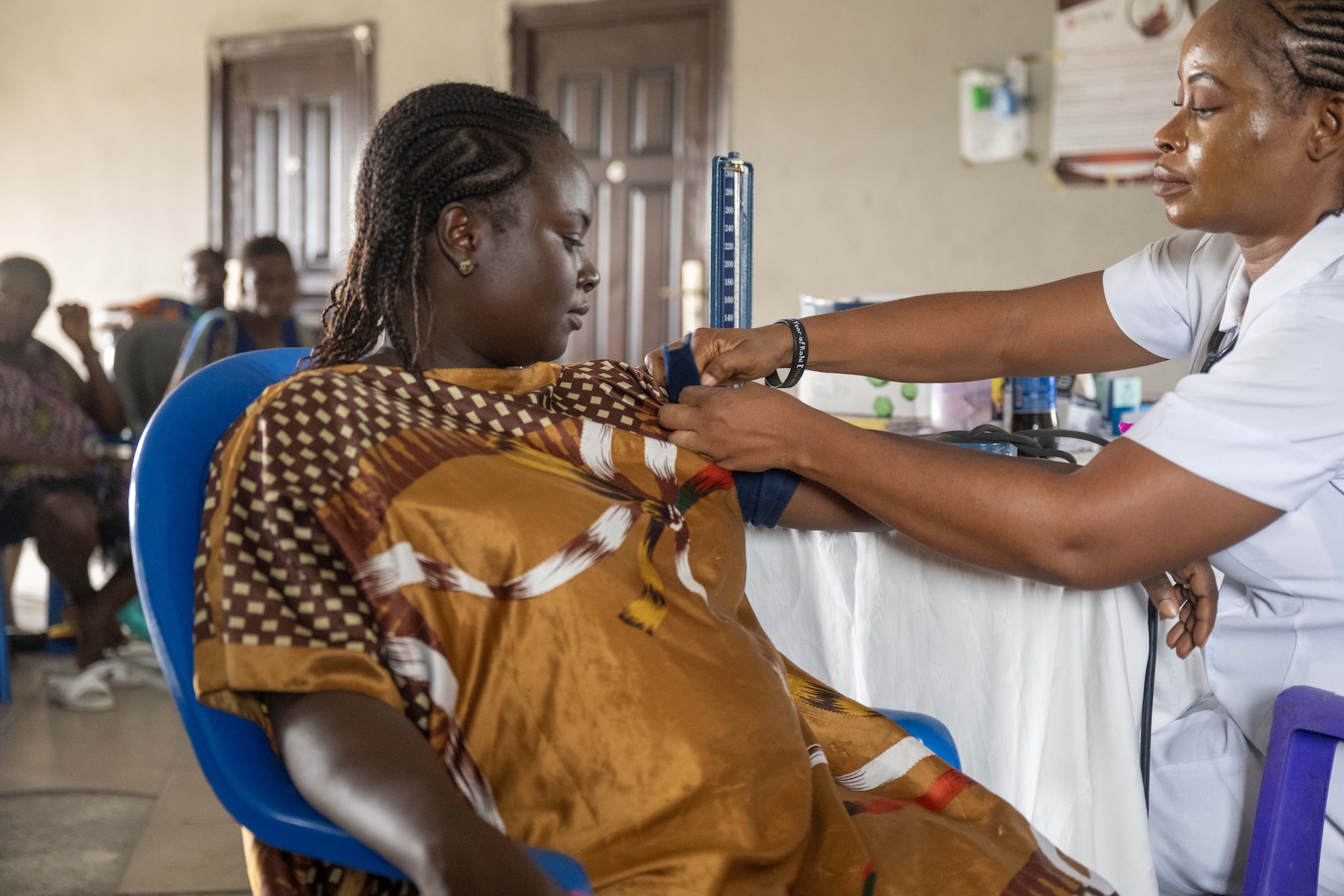
“I really love coming to the antenatal clinic because of the singing,” says Dr. Umahi. “And because the songs have important messages, these clients will remember those messages when they are later humming at home. So it is not just a song.
“Women often feel isolated when they are going through pregnancy,” he continues. “These sessions are designed to build community. With the songs, everybody gets to relax and laugh. Soon, the women are talking to the woman next to them: ‘What is your name? How many months are you? Where do you live?’
“They get support, and they support each other, and it is not so scary to be getting tested and going through the examination, and talking about HIV and other concerns you might have for your child. And they will return for their follow-up appointments because it was an enjoyable experience, and they will get to see their new friends.
“Ending AIDS in children means keeping them safe when they are in the womb,” says Dr. Umahi. “These sessions lead to fewer babies in Okrika born with HIV,” which pays dividends in terms of health; in terms of anxiety and despair; and in terms of cost to the family, the hospital, and the community.”
Today Is a Happy Day
Today Is a Happy Day
Along with the expectant mothers, one new mother, Dorcas, has brought her 6-week-old son, Stephen, to the hospital for early-infant diagnosis—testing the newborn for HIV.
A community health worker, Florence Bapakaye Lawrence, accompanies Dorcas through the procedure. Florence is, herself, living with HIV and has a 14-year-old daughter who is HIV-free. Her role at the hospital is as a mentor mother, to counsel, encourage, and support other women living with HIV.
“I share my experiences with them—because most of them, they don’t like opening up,” says Florence. “These women have a lot of challenges in their lives, but when you open up yourself to them, using yourself as an example, they will be able to open up to you.”

Florence met Dorcas when Dorcas was three months pregnant. Dorcas is living with HIV and knew about her diagnosis, but she had stopped taking her medication because she did not understand that HIV is a lifetime condition. The ARVs had effectively cleared her symptoms, so she stopped taking them. This endangered both Dorcas and her unborn child. Although Dorcas was reluctant to begin taking her ARVs again, Florence counseled her on restarting.
“I gave her a proper counseling,” said Florence, explaining to Dorcas that HIV is different than other illnesses. “I pursued her. I did home visits. I called her on the phone to know how she’s faring, to know if she is taking her medication or not.”
Florence succeeded in bringing Dorcas back to care and followed up with her throughout her second and third trimesters until, finally, Stephen was born. Now it is six weeks later, and they will find out if he has any detectable level of HIV.
The atmosphere is tense. Florence remembers the worry that she had for her own daughter after she was born and is able to assure Dorcas that no matter how the test turns out, things will be OK. If young Stephen tests positive for HIV, he can be put on treatment immediately and remain a healthy and growing child. But there is a good chance that he is HIV-free because Dorcas got back on her medication in time.

Stephen is not too happy. The test requires a blood sample from his foot, and he indignantly yowls in his mother’s arms as the laboratory scientist collects a few crimson drops. In the past the sample would be sent away to a lab, but technological innovation and opportune funding have placed a GeneXpert system right there in the hospital, which can quickly determine whether Stephen is negative or positive for HIV. The laboratory scientist retreats into the lab, and Dorcas and Stephen head to the waiting room.
“Before they started using the GeneXpert machine for early infant diagnosis, it sometimes took two months to get results,” says Dr. Umahi. “By the time the results are back, some of the children had died. Now the woman gets to know the result of her baby’s test before she leaves the facility, and the child can immediately be put on treatment if the test is positive.
After several minutes, Florence comes out to deliver the news: There is no sign of HIV in Stephen. Dorcas finally breaks into a smile of relief. The ARVs did their job!
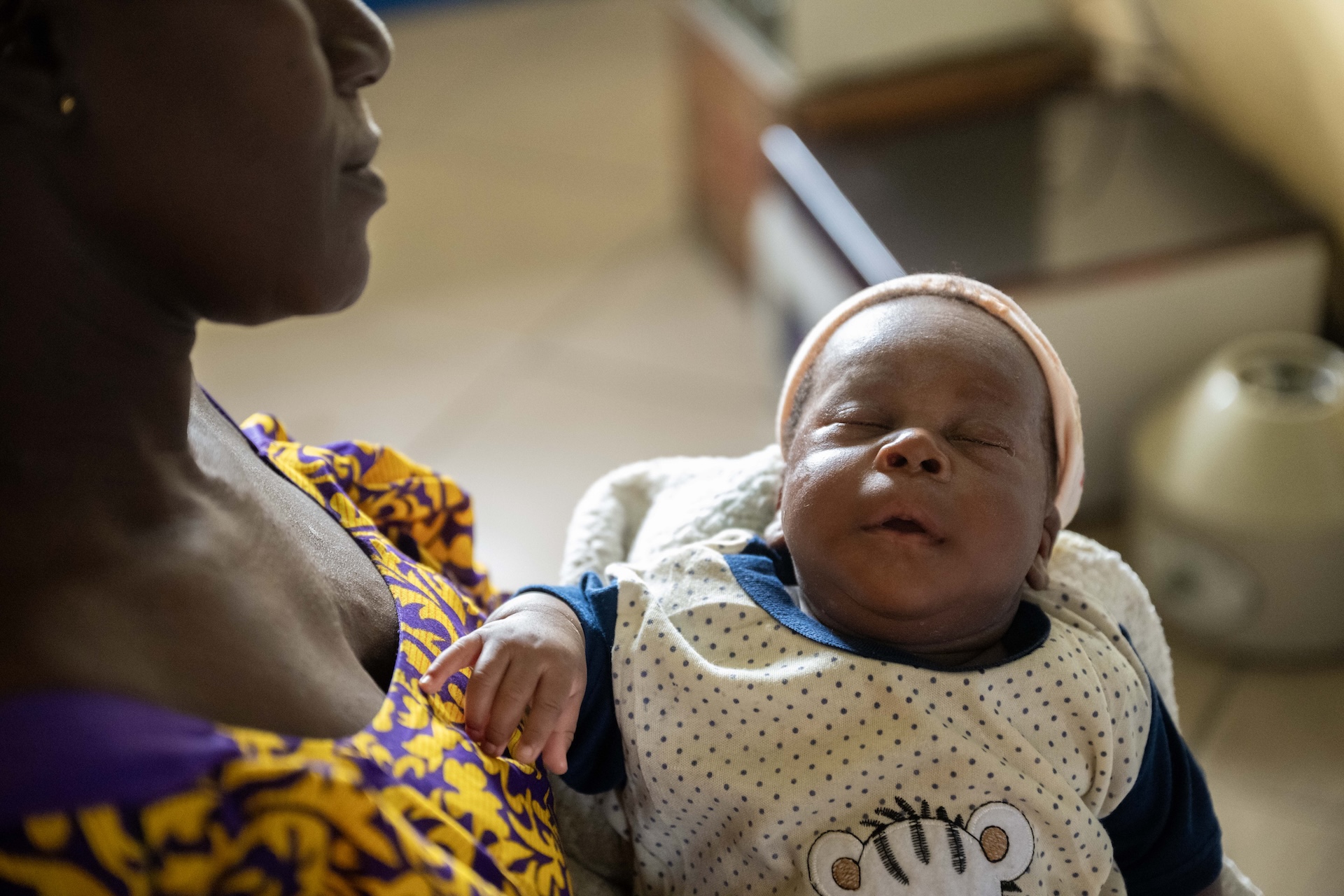
Next, Dorcas is tested to see if her own viral load remains undetectable. Again, good news. Dorcas will be able to continue breastfeeding Stephen as long as she adheres to her drug regimen. Stephen will be tested at periodic postnatal appointments over the next two years—just to be sure.
Florence sweeps up Stephen in her arms and escorts her friend Dorcas through the hospital doors.
“Today is a happy day,” says Florence.
There Is Love in Sharing
There Is Love in Sharing
Florence brings us to meet another one of her clients, Amaka, who has come to the hospital with her 2-year-old son, Emmanuel, for a check-up. It is likely that Emmanuel is alive today only because of Florence’s persistence.
Hospital staff had realized that some mothers in the community were not going through antenatal care and were not bringing their children in to be tested. Florence helped identify 58 infants born to mothers living with HIV who had not been tested. Amaka was one of those mothers. Emmanuel was 11 months old at that time.
“We called her, and she said she didn’t have transportation,” says Florence. “So we found some funding through EGPAF, and we were able to bring her to the facility for tests. We found out that the child was positive.”
“They advised me to start taking the drugs,” says Amaka, and they told me that this is not the end of life [for Emmanuel]. My son will be okay now.”
“So, we immediately started the process of enrollment, where the child got to meet with the doctor. The child got the infant care for HIV,” says Florence.
Emmanuel is now connected to the hospital, and his mother makes sure that he takes his ARV medication daily so that he will stay healthy and live a normal life. He likes to practice his ABCs and watch cartoons. He will be enrolling in school shortly, says Amaka.


Florence says that she loves her job as a mentor mother—especially when she can change the outcome for a child, like Emmanuel.
“These women are struggling, like every other woman in the community,” says Dr. Umahi. “But in addition to the struggling, now she has a life-changing diagnosis.
“These women have to wake up at 6 a.m., prepare their children to go to school and then head to the market where they trade or maybe they go farming or fishing to provide for the family. So doing all that sometimes you don’t remember that you need to take care of yourself because you are swallowed up in the complexities of life.
“The mentor mother helps in providing that level of reminder. The mentor mother calls to ask ‘How are you? Have you taken your medications today? Is there anything you need? How is your child? Do you want us to meet?’
“The mentor mother knows what she is going through and the other mother can confide in her because it’s not everyone that she shares her HIV diagnosis with. This is not something that she will talk about with other women in the marketplace.
“And this becomes even more complicated if you also have a child living with HIV, who needs to be taking medication and tested for viral load. Sometimes women don’t want to share this information with other family members; you see women chased out of their marriage because of an HIV diagnosis,” says Dr. Umahi.
Florence says that she appreciates the close bond that she forms with her clients.
“There is love in sharing. You can share with a friend everything about you, things that you cannot share with your husband,” says Florence.
We Decided to Bring It to One Hundred Percent
We Decided to Bring It to One Hundred Percent
Finally, we came to see Dr. Lilian Anunobi, M.D., the ART doctor at Okrika. She allowed us to sit in with her as she attended to Minfaka and her 1-year-old daughter, Derefaka. This mother and baby provide proof of concept when it comes to reaching Generation Zero—no child born with HIV. The mother, Minfaka, is living with HIV and went through the antenatal and counseling process. She has adhered to medication, and her daughter is HIV-free.
Aside from a confirmatory test to ensure that Derefaka remains HIV-free, this is a routine pediatric check-up. Dr. Lilian says that she hopes that eventually all of her young patients will be like Derefaka.


A relative newcomer to the facility, Dr. Lilian realized that many mothers and children in the community were not being seen regularly at the facility. Simply waiting for clients to walk in meant that many HIV-affected children were not being tested, with tragic consequences. Dr. Lilian decided that the hospital could not ignore the children in the community who were in danger of dying.
After attending several EGPAF-supported workshops on quality improvement—a continuous process for systematically identifying gaps in the health system and problem solving to close those gaps—Dr. Lilian took action.
“I called my team, and we started listing the areas that we have problems in the hospitals. And we found out that in our list, early infant diagnosis has a low testing rate—that people are not really accessing it.
“We are at zero percent from our child follow-up register [meaning that the only children being tested were those whose mothers walked in for their appointments]. So we decided to bring it up from zero percent to one hundred percent within one month.
“We have areas around the creek and the fishing pond where people settle. It is a remote area, so it requires a lot for people there to come to the hospital. Sometimes they have to charter a canoe,” Dr. Lilian says.
“So, what do we do? We decided to start by tracking each patient. We send them SMS [text messages] or call them on the phone,” says Dr. Lilian. “After that, we do home visits, especially to those people living in the creek, living in the hard-to-reach areas. We have to go there and test them or bring them to the hospital.

Within one month, the hospital had identified 58 babies with HIV-positive mothers and tested all of them.
“After doing this, we had one HIV-positive child [Emmanuel], whom we have enrolled into care. So, he’s receiving care. He’s doing well,” smiles Dr. Lilian.
Babies of Hope
Babies of Hope
Dr. Umahi says that the babies we have met today at Okrika represent hope for eliminating HIV in this community. It starts with the children, he says.
“A fetus that is still in utero doesn’t know the realities of life. And here is the mother who is trying to make every effort to protect her baby from becoming HIV-positive. Her hope while she is pregnant is to make a healthy future a reality for her child.
“There is another baby that has been delivered, and the mother is coming to check his HIV status: ‘Have I succeeded in preventing mother-to-child transmission?’ She is worried before the test, but she walks away with her hope renewed.
“Then, there is the baby who slipped right through the crack—but the facility went back to their data and was able to notice that he had not been diagnosed, and that baby was found. If not for that intervention, there wouldn’t have been hope because the baby would have been lost.
“And the last is a child growing up HIV-free and has come with her mother to be seen by the doctor and have a comprehensive health check.
“So how do we renew hope?” asks Dr. Umahi. “By providing comprehensive care that is needed at the different stages of a child’s life so that they’re able to grow and live and become who they want to be.”

“How do we renew hope? By providing care that is needed at the different stages of a child’s life so that they’re able to grow and live and become who they want to be.”
Dr. Umahi Godwin




